We will have to wait to find out if audits will lessen now that the new pricing structure has dramatically decreased the monetary incentive for audits.
Blog Posts About Regulatory Updates
An Update on the CAMPS Legal Initiative to Reverse Skin Substitute Payment Pricing – Guest Blog by Dr. Ryan Mathis
The deadline for the CAMPs Initiative to appeal the court’s decision was May 11, 2026. Here’s an update about what happened by Dr. Mathis.
UnitedHealth and CVS Health Announce Progress Toward Standardizing the Process for Prior Authorization Requests
UnitedHealth and CVS Health announced that they have standardized data and submission requirements for more than half their prior authorizations (PAs).
CMS Launches Newsletter to Help Small Practices (15 or Fewer Clinicians) Understand MIPS and the Quality Payment Program
2026 is the 6th year that practitioners could lose up to 9% of their Medicare claims under MIPS.
TMA Raises Awareness About Drug Access Limitations by Pharmacy Benefit Plans – Guest Blog by Dr. Jay Shah
Dr. Jay Shah, President of the Texas Medical Association (TMA) has provided this guest blog about what the TMA is doing to monitor the issue of pharmacy benefit plan limitations on drug access.
Trouble with Medicare “Dis” Advantage Programs? CMS has a Provider Complaint Form
The update represents a formalized mechanism for providers to raise concerns directly with CMS regarding Medicare Advantage plans.
Telehealth & Remote Monitoring Billing & Payment
CMS released an updated Medicare Learning Network (MLN) publication outlining 2026 changes.
New Medicare Advantage Complaints Process
On December 22, 2025, CMS implemented an online form on cms.gov for providers that need to report a complaint about a Medicare Advantage plan.
Off-Campus HOPDs Need a Separate NPI – Is This a Prelude to Site Neutrality? (Guest Blog by Dr. Helen Gelly)
MEDPAC has been recommending site neutrality for decades, and perhaps the powers that be at CMS are listening.
How is Medicare Prior Authorization Going for You Under WISeR in Texas? Dr. Shah of the TMA Wants to Know!
This is a rare and wonderful opportunity to have your voice heard by a powerful state medical association (with a president who is a wound care expert!)
How a Non-Pressure Ulcer Cost Measure Could Help or Hurt Your MIPS Score (and Your Medicare Payments)
CMS is going to create a wound-relevant cost measure no matter what. Let’s make sure it is as accurate and fair as possible.
Part One of My Interview on CTP Changes is Now Available on HMP Global Learning Network/Wounds
On Jan. 8, 2026, HMP posted the first part of my interview on “The Impact of CTP Changes on Provider Types.”
Texas Medical Association (TMA) resources for the new WISeR prior authorization program affecting CTP/skin subs
The Texas Medical Association (TMA) has a new education sheet to guide clinicians through services...
In 2026, Monetary Threshold is Higher for Medicare’s Expedited Access to Judicial Review (EAJR)
I hope those of you who are experts at the appeals process will provide some information in a guest blog about the EAJR process.
Step-by-Step Instructions on How to Download Your Field Test
CMS has posted the Cost Measure Field Test reports on the QPP website! It’s time for you to download yours!
CMS Press Release: Prepare for 2026 Field Testing of Episode-Based Cost Measures
Field Test Reports for eligible clinicians and clinician groups will be available on the Quality Payment Program Portal beginning January 29.
How to Prepare For & Make the Most of Your Field Test – Attend CMS Meetings on Jan 27 and Feb 18
CMS is holding office hours with specialty societies and organizations to provide information about the upcoming field testing period.
Here We Go Again: CMS is Testing a New “Non-Pressure Ulcer” Cost Measure
I will be posting a series of blogs explaining this in more painful detail, including a step by step guide to download your Field Test report.
Noridian Webinar Materials on Wasteful and Inappropriate Service Reduction (WISeR) Model
I attended the Noridian informational call on the Wasteful and Inappropriate Service Reduction (WISeR) model.
Breaking News! Medicare Will Not Pay for CTP / Skin Substitute Wastage “Under Any Circumstances”
Medicare fee for service (FFS) does not pay for discarded amounts of “incident to supplies” (which is how all non-BLA CTPs/skin subs are now classified) and will only pay for the amount of product furnished.
A New Era for Cellular Tissue Products / Skin Substitutes
Price controls are better for patients, Accountable Care Organizations, secondary insurers, tax payers, and the Medicare trust fund.
Breaking news! Cellular Tissue Products (CTPs) / CAMPS to be Paid at $127.28/cm2
Breaking news! Physician fee schedule finalized: CTPs/CAMPS priced at ~$127.28/cm2. Read more...
Cellular Tissue Products / Skin Substitute Applications in the Home Setting – Check Out Kathleen Schaum’s Recent Article in Advances in Skin and Wound Care
The application of a Cellular Tissue Product (CTP) / skin substitute, a surgical procedure, is out of the scope of a registered nurse.
Practitioners May Now Review Their 2024 Merit-Based Incentive Payment System (MIPS) Final Scores
To address errors with the 2024 MIPS final scores, CMS says participants have approximately 60 days to request a targeted review.
Check the OIG list of “Excluded Individuals” Before Hiring!
To avoid CMP liability, health care entities should routinely check the list to ensure that new hires and current employees are not on it.
Dear APM Docs: Your 2023 APM Bonus Is Waiting… If CMS Can Find You
You might be participating in an APM and not even know it – that happens a lot – so there’s no harm in updating your payment information.
2024 MIPS Final Scores Won’t Publish Until Fall
Download the 2024 MIPS scoring guide for more information on performance criteria and how final scores are calculated.
CMS Warns of Fraud Scheme Around Medicare Audits
CMS has identified a fraud scheme targeting Medicare providers and suppliers. If you receive a suspicious request, don’t respond.
DEA Warning: Fraudsters Impersonating DEA Officials are Scamming Clinicians
Federal law enforcement officers are prohibited from demanding cash or gift cards from a member of the public.
Hyperbaric Physicians (and Hospital Program Managers): Check the 2023 Medicare Data! Protect Your NPI and Don’t Put Hospital Facility Fees at Risk
Check the 2023 Medicare data! Protect your NPI and don’t put hospital facility fees at risk.
Just Released: Hospital Outpatient Proposed Rule Would “Unbundle” Cellular Tissue Products (CTP) / Skin Substitutes in the HOPD
I will try to post a better analysis of the impact of these proposals in the HOPD (hopefully provided by readers who understand this better than I do).
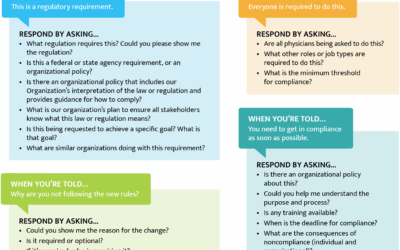
Show Me the Regulation!
When clinicians or management companies ask why a process must be done in a certain way, they are told, “It’s a regulatory requirement.”
BREAKING: 2026 MPFS Proposed Rule sets single payment for all CTPs at $125.38/cm2
There will no doubt be a significant response from manufacturers and clinicians in response to this proposal.
RFK Jr. and Dr. Oz Pledge to Fix Broken Prior Authorization System
heir commitments reinforce the role of CMS in monitoring outcomes and promoting accountability.
BREAKING NEWS in the DOJ Press Conference! More Skin Substitute / Cellular Tissue Product (CTP) Fraud Indictments
Wound Care, specifically around the use of amniotic “skin substitutes,” made the news in the fraud press release.
Site Neutrality – a Looming Disaster or an Opportunity?
Now may be the time for academic programs and large hospital systems that still provide needed emergency hyperbaric services to start contacting their congressmen.
The Quality Payment Program (QPP) “Doctors and Clinicians Preview Period” for 2023 is Officially Open
Clinicians who reported data as part of the Quality Payment Program (QPP) in 2023 can preview their 2023 performance information before it appears on the Medicare.gov compare tool and in the Provider Data Catalog (PDC).
DOJ Unveils a New Corporate Enforcement & Voluntary Self-Disclosure Policy (CEP)
The Department of Justice’s Criminal Division is “turning a new page on white-collar and corporate enforcement.”
Providers Under Siege
The stakes go beyond money: reputational harm, exclusion from Medicare and Medicaid, and even criminal charges are on the table.
States Try to Limit the Use of AI in Prior Authorization
Read the complete article for more details on what individual states are doing to push back on the use of AI in Prior Authorization.
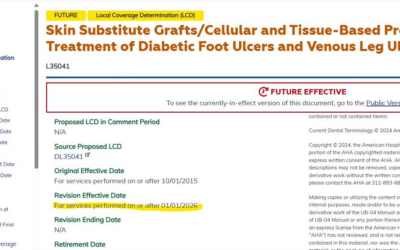
CTP-related LCDs Postponed at the Last Minute!
The LCDs that will directly impact CTPs (Skin Subs) have been postponed until January 1, 2026! Announcement came at the last minute!
Overzealous Medicare Audits
Be sure to read all of Ms. Emanuel’s article, which calls for radical reforms such as holding auditors accountable for mistakes.
What Happened to “Innocent Until Proven Guilty? Check Out this Article on Medicare Recoupment
Check out Knicole Emanuel’s recent blog post about CMS monetary recoupment before full adjudication.
Fewer Regulatory Hoops but Continued Scrutiny on Fraud Under the Trump Administration
While the Trump Administration may be reducing the regulatory burden in many areas of government, they are NOT reducing their focus on reducing on fraud investigations.
ACA Healthcare Plan “Just Say No” to 1 in 5 Claims
ACA insurers denied 1 in 5 medical claims in 2023, the highest rate since 2015.
Murphy Introduces Bipartisan Legislation to Preserve Medicare for Patients and Physicians
I worry that the misbehavior of a small percentage of practitioners will reduce enthusiasm for a bill to fix a huge physician reimbursement problem.
A Titanic Shift at CMS: The Push to Trim Administrative Costs & Increase Audits – Knicole Emanuel’s Recent Post
Ms. Emanuel likens CMS to the Titanic in terms of how hard it will be to turn such a massive ship. Let’s hope this story will end differently.
“Defending Against Medicare and Medicaid Audits: A Guide for Healthcare Providers” by Knicole Emanuel
She notes that, “Recent statistics show that CMS, through its contractors, conducted over 300,000 audits in recent years.”
Noridian Surgical Dressings Webinar – 02/11/2025
The Noridian Provider Outreach and Education staff is hosting the Surgical Dressings webinar on 02/11/2025, 12:00 PM – 1:30 PM EST.
Landmark Antitrust Settlement Calls for Blue Cross Blue Shield to Pay $2.8 Billion into a Fund Designated for Physicians and Others
The fund is designated for settlement class members, including physicians, group practices, and health care facilities.
LCDs Delayed Until April 13, 2025
If you scroll to the end of the LCD, it will state the future effective date of 4/13/25.
American Relief Act Extends Some Telehealth Waivers Including Audio-Only Telehealth
The continuation of Medicare telehealth flexibilities follows another recent telemedicine extension by the DEA and the Department of HHS.
BREAKING NEWS: Wound Care Company Owners Plead Guilty to $1.2 B in Fraudulent Claims for Amniotic Products and Face Prison
The case was handled through the Health Care Fraud Strike Force Program, which currently operates in nine Strike Forces across the country.
Physicians Have Concerns Over the Implementation of Medicare’s Add-on Code for Complex Care (G2211)
The rules are complex, and a billing and coding expert may need to provide guidance to wound care practitioners.
Changes to the Administrative False Claims Act (AFCA) Mean That “Smaller” Medicare Fraud Cases (Up to $1 Million) Can Be More Easily Prosecuted
This legislation also makes it more likely that individuals who act as “whistleblowers” could realize the associated monetary rewards.
The New LCDs are (Almost Certainly) Coming to Town
I may post more information about the meeting later, but the general tone of the MAC medical directors was confident.
AMA sues MultiPlan Alleging Price-Fixing for Out-of-Network Physician Payments
The American Medical Association (AMA) and the Illinois State Medical Society (ISMS) have filed a lawsuit in federal court.
CMS Releases the Medicare Physician Fee Schedule Final Rule for 2025
The sad news is that CMS is going ahead with a 2.9% cut to Medicare physician reimbursements for 2025.
ICD-10 Changes
There were 252 new codes added, 36 code deletions, and 13 code revisions effective October 1, 2024.
CMS Releases 2025 Final Rule for the Hospital Outpatient Prospective Payment System (OPPS)
The short version, based on my cursory read, is that no old problems were fixed but no new problems were created by the final rule.
Breaking News! LCDs for Cellular Tissue Products / Skin Substitutes Released!
LCD – Skin Substitute Grafts/Cellular and Tissue-Based Products for the Treatment of Diabetic Foot Ulcers and Venous Leg Ulcers (L39756)
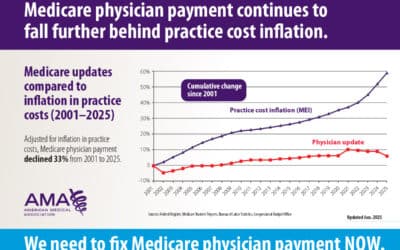
Bipartisan Bill Introduced That Would Provide a 4.7% Medicare Physician Payment Update
It would eliminate the 2.8% Medicare physician payment cut and provide a positive update that equals half of the Medicare Economic Index.
“To Self-Disclose or Not to Self-Disclose”: Check Out Attorney Knicole Emanuel’s Blog
Self-disclosure is better than waiting to get caught. Lives can be ruined if you wait to get caught.
Templated Notes and Medicare Audits
If practitioners encounter denials by auditors based on the use of note templates, they should probably seek legal counsel.
Reminder: Final Scores for the 2023 Performance Year of Medicare’s Merit-Based Incentive Payment System (MIPS) are Now Available Online and the Deadline to Request a Review is October 11 at 8 PM ET
Check your scores soon as they will impact your 2025 Medicare payment!
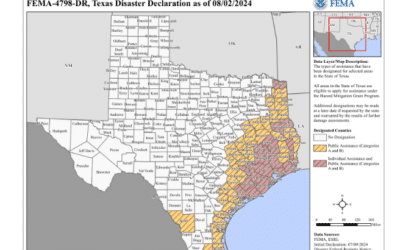
Due to the Impact of Beryl, CMS Has Automatically Applied a Hardship Exemption Within the 2024 Merit-Based Incentive Payment System (MIPS) Performance Period to Eligible cC Areas
The extreme and uncontrollable circumstances (EUC) policy will apply in affected Texas counties as identified by federal public health emergency and disaster declarations.
Check Out the New Article in TWC “I’m Getting Audited – Now What?” by Stephen Bittinger
Mr. Bittinger’s article explains the various types of audits, what’s at stake, and how an attorney might help.
Aetna to Cut Payment for Urgent Care Surgical Services and Payments for NPs and PAs
Wound Care practitioners who bill site of service 49 (independent clinic) take note!
In 2025, Physicians Face a 2.8% Pay Cut While Mandatory Participation in an MVP Looms
In 2024, physicians had a 1.68% pay cut and they remain the only Medicare providers to not receive an inflationary update.
Noridian and CGS Release FAQs on Lymphedema Compression Treatment Items
Noridian and CGS Provider Outreach and Education have released the most frequently asked questions (FAQs) on lymphedema compression treatment items under the Lymphedema Treatment Act.
Health Information Technology Proposed Rule (HTI-2) is Out
ONC will be hosting information sessions in the coming weeks, including an overview session on July 17 at 2:00 PM ET.
2025 Medicare Physician Fee Schedule is Out (and CMS Did Not “Package Price” Cellular Tissue Products / Skin Substitutes in the Doctor’s Office)
The billing of CTPs in the doctor’s office is unchanged. The 2025 Medicare conversion factor is set to decrease for the fifth straight year.
Breaking News! OPPS Proposed Rule is Out!
At first glance, there are no changes to Cellular Tissue Product /skin substitute payment, which remain under package pricing in this site of care.
Accelerated and Advance Payment (AAP) for Medicare Ends on July 12
CMS announced that Medicare payments under the Accelerated and Advance Payment (AAP) Program for the Change Healthcare/Optum Payment Disruption (CHOPD) will end on July 12.
CMS Adds 76 New Items to its Master List of DME Supplies That May Be Subject to Prior Authorization (and Some Surgical Dressings are on the List)
The Centers for Medicare & Medicaid Services (CMS) added 76 new items and deleted three from its master list of durable medical equipment (DME), prosthetics, orthotics, and supplies.
Skin Substitute Proposals: What You Can Do
These proposals are in a comment period until June 8, 2024. Any interested stakeholder may submit comments to share their feedback on these proposals.
Pneumatic Compression Devices Are in the Spotlight for 2024 Audits
Check out the article by Knicole Emanuel in Today’s Wound Clinic: Pneumatic Compression Devices Are in the Spotlight for 2024 Audits.
CMS Explains its 2024 Value-Based Care Strategy
CMS ALWAYS tell us what they are going to do before they do it. Then they do it, and we are surprised.
A Little Reprieve for Physician Pay Cuts
A 3.4% Medicare physician pay cut took effect on January 1, 2024. However, thanks to the passage...
MIPS Quality Measure #130 Documentation
Too many providers are under the impression that merely documenting the patient’s medication list satisfies the performance of this measure, and it does not.
CMS Announces Flexibilities in the Wake of the Change Cyberattack
CMS is encouraging MA plans to offer advance funding to health care professionals most affected by the cyberattack.
CMS Announces Reopening of 2023 MIPS EUC Application in Response to Change Healthcare Cyberattack
I am reposting the entire message from the CMS about the extension of the Extreme and Unavoidable...
CMS Removes the Requirement for AUC From the 2024 Medicare Physician Fee Schedule
Implementing the AUC program would have been a time consuming and expensive lift for practitioners.
Update on the Surgical Dressing Policy – Thanks to the Alliance of Wound Care Stakeholders
The Alliance of Wound Care Stakeholders has had another policy win!
Resources from CMS and the AMA to Help You Implement Changes to Physician Documentation & Billing
There have been two major changes in the regulations pertaining to physician documentation during ambulatory visits, both of which are favorable for wound care practitioners.
Medicare Audits on Pneumatic Compression & Surgical Dressings – “It’s About the Documentation…”
I am a huge fan of attorney Knicole Emanuel’s blog and her most recent post is directly relevant to the field of wound care.
Be Careful Billing the New CMS G2211 Add-on Code for Visit Complexity
It is intended to “better recognize the resource costs associated with evaluation and management visits for primary care and longitudinal care.”
Noridian Has Begun Requesting “Documentation to Support Credentialing of the Provider Performing the HBO Service”
If there are super-secret requirements that Noridian has now decided to impose, then they should be enshrined in a public document somewhere.
CMS Final Rule on Prior Authorization Released
Prior authorization (PA) is costly, inefficient and responsible for patient care delays. The...
The Deadline to Submit MIPS Data for 2023 is April 1 at 6 pm EST to Avoid up to a 9% Penalty on Medicare Revenue
The data submission period for Medicare’s Merit-Based Incentive Payment System (MIPS) 2023 performance year is underway.
Time Sensitive! It’s Not Too Late to Sign the Letter to CMS Protesting the 41.5% Reduction of HBOT Facility Fees!
I know the holidays are busy – but most of us would like to have a job to go back to in January…
Without Warning – the Outpatient Prospective Payment Final Rule Cuts HBOT Facility Fees by 40%
What we need is for people to submit a comment, and to spread the word that hyperbaric oxygen therapy is in a crisis.
ICD-10 Changes
A new ICD-10 Clinical Modification (ICD-10-CM) code set took effect October 1, 2023. In this new code set, there are many code additions, deletions, and modifications.
Modifications Needed to Wound Center EHR to Support DME Orders for Dressings
Your EHR will need to be modified to meet the DME documentation requirement burden (and if you think the list below is ridiculous – it is, but it’s still required).
JZ Modifier Use With Skin Substitutes
CMS has issued guidance requiring the use of Modifier JW on all claims for biologicals from single-dose containers that are separately payable under Medicare Part B when there are unused / discarded amounts.
Observations About the 2024 PFS Pertaining to Cellular and/or Tissue-Based Products in the Doctor’s Office Setting
On July 13, 2023, CMS issued proposed rules for the 2024 Physician Fee Schedule (PFS) and the Hospital Outpatient Prospective Payment System (OPPS).
“Hidden RAC Audits” – Seriously…
Attorney Knicole Emanuel has posted a chilling blog on her site about hidden RAC (Recovery Audit Contractor) audits.
Ulcer Debridement & Total Contact Cast Application
We cannot submit CPT®[1] coding for both ulcer debridement and total contact cast application when both are performed for the same ulcer at the same encounter.
Listen to a Podcast with Dr. Helen Gelly, “How to Get Your Wound Clinic Through an Audit”
On your drive home, check out this podcast with Helen Gelly MD, FUHM, FACCWS, UHM/ABPM, “How to Get Your Wound Clinic Through an Audit.”
HBOT Facility Payments are Under Attack (Physician Supervision is Next…)
We need individuals at all training levels to comment on the proposed changes that CMS is proposing in the Medicare Physician Fee Schedule (MPFS) for the technical payment of HBOT.